Dental sleep medicine is a branch of dentistry that treats snoring and obstructive sleep apnea with custom oral appliances as part of a physician-led care plan. If you have seen the term and felt unsure what it actually means, you are not alone. Many people confuse it with sedation dentistry or cosmetic marketing language. In reality, it is a structured, guideline aligned branch of care that works alongside medical sleep providers.
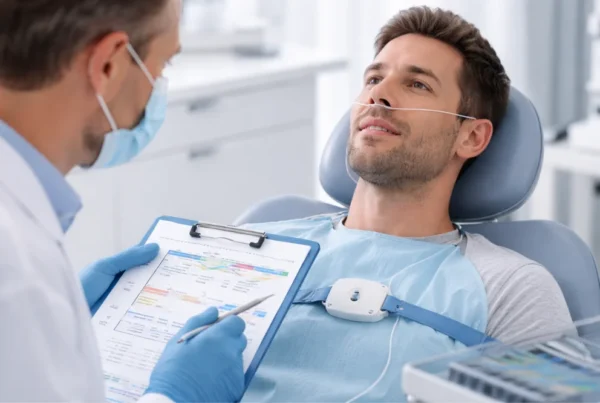
At Airway Dentistry DHS, patients from Palm Springs, Cathedral City, and Rancho Mirage often ask how a dental office fits into a medical sleep diagnosis. Dr. Juana Cavinder DDS, MPH combines more than 30 years of clinical dentistry with advanced airway focused training. That matters because sleep apnea is a medical condition, yet the structures that influence it live inside your mouth. When medical and dental care are coordinated clearly, patients feel supported instead of confused.
What Exactly Is Dental Sleep Medicine?
Dental sleep medicine focuses on the oral and maxillofacial aspects of sleep related breathing disorders. It addresses conditions such as snoring and obstructive sleep apnea by evaluating jaw position, tongue posture, and airway space. When those structures contribute to airway collapse during sleep, dental interventions can help stabilize breathing. The work happens within a broader medical plan, not outside of it.
This field is supported by professional academies and defined clinical standards. Dentists who practice it typically pursue additional training beyond general dentistry. That training focuses on airway anatomy, appliance design, titration protocols, and long term bite monitoring. The goal is measurable improvement in breathing, not simply reducing snoring volume.
How Dental Sleep Medicine Fits Into Medical Sleep Care
Dental sleep medicine does not replace your sleep physician. A medical sleep specialist diagnoses obstructive sleep apnea through a sleep study and determines severity and systemic risk. Once diagnosis is confirmed, the physician may prescribe oral appliance therapy as an alternative or complement to CPAP. The dentist then designs, fits, and adjusts the appliance under that prescription.
A simplified care flow often looks like this. The dentist screens for airway risk during a routine exam and refers for a sleep study when symptoms are present. The physician confirms diagnosis and recommends therapy options. If an oral appliance is appropriate, the dentist provides and titrates it, then communicates results back to the physician for follow up testing and long term oversight.
Core Tools: Oral Appliance Therapy and Related Care
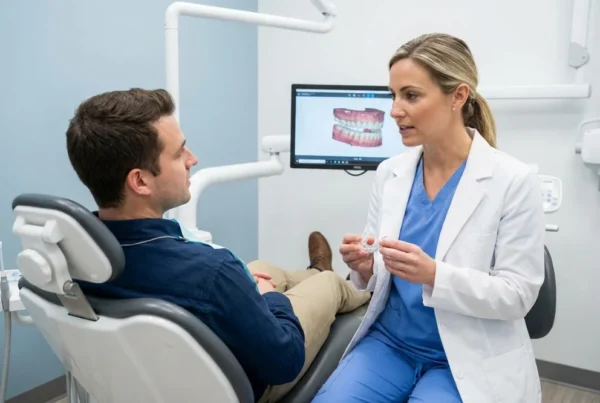
Instead of pushing air into your airway like CPAP, an oral appliance changes the shape of your airway from the inside. It gently advances the lower jaw forward during sleep, helping prevent the tongue and soft tissues from collapsing backward. This approach is commonly used for mild to moderate obstructive sleep apnea and for people who cannot tolerate CPAP masks. Modern appliances are custom made and adjustable for comfort and effectiveness.
Digital scans and 3D workflows allow greater precision than older impression techniques. Dentists also monitor jaw joints, tooth position, and muscle comfort over time. That ongoing care distinguishes dental sleep medicine from generic over the counter snore guards.
To understand how oral appliances compare to CPAP at a high level, consider this overview.
| Feature | Oral Appliance Therapy | CPAP Therapy |
| Mechanism | Repositions the lower jaw to support the airway | Delivers continuous air pressure through a mask |
| Best suited for | Mild to moderate OSA or CPAP intolerance | Moderate to severe OSA |
| Portability | Small and travel friendly | Requires machine, tubing, and mask |
| Monitoring | Dental follow up plus physician oversight | Physician oversight and device data |
Both therapies have value, and the right decision depends on apnea severity, anatomy, and what you can realistically use every night. Consistent use often matters as much as theoretical effectiveness.
Who Is a Good Candidate for Dental Sleep Medicine?
Dental sleep treatment works best when airway anatomy, dental stability, and overall medical profile align for success. Many adults with diagnosed mild to moderate obstructive sleep apnea respond well to oral appliance therapy when it is properly prescribed and monitored. Patients who struggle with CPAP comfort may also be appropriate candidates if medical supervision continues. The decision is always individualized and based on both dental findings and physician input.
- Adults with diagnosed mild to moderate obstructive sleep apnea
- Individuals who cannot tolerate CPAP but remain under physician care
- Frequent travelers who need a portable and quiet therapy option
- Patients whose jaw position contributes to airway narrowing
Final candidacy decisions are made jointly between the sleep physician and the dentist after reviewing severity, anatomy, and long term health considerations. Dentists evaluate jaw mobility, tooth stability, and TMJ health before recommending an appliance. Physicians continue to monitor medical risk and apnea control through follow up testing.

Benefits and Risks You Should Understand
Like any medical treatment, dental sleep medicine has advantages and trade offs. Many patients prefer a compact, non-invasive device that does not involve a mask or machine. Portability makes travel easier and nightly setup simpler. For some people, comfort improves adherence compared to CPAP.
There are also risks that must be discussed honestly. Temporary jaw soreness, tooth sensitivity, minor bite shifts, or TMJ flare ups can occur. Regular follow up visits allow early adjustment and reduce long term complications. Ignoring discomfort rather than addressing it increases risk.
Objective follow up testing remains essential. Feeling better is encouraging, but a repeat sleep study confirms whether apnea severity has actually improved. Responsible care always includes monitoring rather than a one time fitting.
What to Expect at a Dental Sleep Medicine Visit in 2026
Your first visit focuses on understanding your sleep history and goals. Your sleep study, medications, and symptoms are reviewed carefully. The dentist evaluates your teeth, jaw function, and airway anatomy. Digital scans are often used to design a precise custom appliance.
- Week 0: Consultation and review of sleep study
- Week 2 to 3: Appliance delivery and instruction
- Month 1 to 3: Gradual titration visits
- Month 3 to 6: Follow up sleep testing with your physician
When the appliance is delivered, it is adjusted for comfort and fit. You receive clear instructions on cleaning and wear schedule. Gradual titration visits fine tune jaw position over time. Follow up testing confirms whether breathing has measurably improved.
Training and Choosing the Right Provider
Not every dentist who mentions sleep has advanced training in dental sleep medicine. Many pursue additional education, mini residencies, or board certification focused specifically on airway and sleep related care. Membership in recognized professional organizations signals commitment to evidence based standards. Experience and physician collaboration matter more than marketing language.
When choosing a provider, ask about training background, case volume, and how success is measured. Ask how often they communicate with sleep physicians and how they monitor bite changes long term. A strong provider welcomes these questions and answers transparently. Safe care is built on clarity rather than convenience.
You Deserve Clear Answers and Coordinated Care
Sleep apnea can feel confusing, especially when you are trying to decide between CPAP, oral appliances, or other therapies. You deserve a plan that respects both medical science and the role your jaw and airway play in breathing. The problem is not who you are, it is a condition that can be addressed with the right guidance. You are the hero of this story, and your role is to choose informed care.
Airway Dentistry DHS serves patients in Desert Hot Springs, Palm Springs, Cathedral City, and Rancho Mirage as part of that coordinated approach. Dr. Juana Cavinder works alongside sleep physicians to provide structured, evidence based oral appliance therapy when appropriate. The path is simple and clear, confirm diagnosis, choose the right therapy, and monitor progress with integrity. If you are ready to explore whether dental sleep medicine belongs in your care plan, schedule a consultation and take the next step toward better rest.
Frequently Asked Questions
Is dental sleep medicine the same as sleep dentistry?
Dental sleep medicine is not the same as sedation or comfort focused sleep dentistry. Sedation dentistry helps patients relax during procedures, while dental sleep medicine addresses breathing disorders such as snoring and obstructive sleep apnea. It focuses on airway anatomy and custom oral appliances within a physician led care model. The distinction matters because one treats anxiety during dental treatment and the other treats sleep related breathing disorders.
Can a dentist diagnose sleep apnea?
A dentist cannot diagnose obstructive sleep apnea because diagnosis requires a formal sleep study interpreted by a medical sleep physician. Dentists screen for airway risk factors and refer patients for testing when symptoms are present. Once a physician confirms diagnosis and prescribes therapy, the dentist provides and monitors the oral appliance. This team structure protects safety and keeps responsibilities clear.
The Role of Dentists in the Diagnosis and Treatment of Obstructive Sleep Apnea
Is an oral appliance as effective as CPAP?
CPAP remains the gold standard for severe obstructive sleep apnea because it delivers continuous air pressure to prevent airway collapse. Custom oral appliances are highly effective for many patients with mild to moderate OSA and for those who cannot tolerate CPAP. Real world adherence plays a major role in outcomes, and some patients use their oral appliance more consistently. The best choice depends on severity, anatomy, and comfort.
AASM and AADSM Issue New Joint Clinical Practice Guideline for Oral Appliance Therapy
Will an oral appliance change my bite?
Minor bite changes can occur over time, which is why ongoing monitoring is essential. Dentists evaluate tooth position, jaw joints, and muscle comfort during follow up visits. Early adjustments reduce the likelihood of significant long term changes. Responsible dental sleep medicine includes supervision rather than unsupervised device use.